Ibogaine & The Heart
Ibogaine is known to effect the heart and not interact well with some other drugs, medicines or pre-existing medical conditions.
On this page we look at studies on the fatalities associated with ibogaine and what has been learnt from this to reduce the risks of future ibogaine treatments. We will look at how ibogaine effects the heart, associated risk factors, the typical arrhythmias seen, and the cardiac monitoring necessary during an ibogaine treatment.
Ibogaine is also anti-addictive in humans as the drug alleviates drug craving and impedes relapse of drug use. Although not licensed as therapeutic drug and despite safety concerns, ibogaine is currently used as an anti-addiction medication in alternative medicine in dozens of clinics worldwide. In recent years, alarming reports of life-threatening complications and sudden death cases, temporally associated with the administration of ibogaine, have been accumulating. These adverse reactions were hypothesised to be associated with ibogaine’s propensity to induce cardiac arrhythmias.
Xaver Koenig and Karlheinz Hilber
Department of Neurophysiology and Neuropharmacology, Medical University of Vienna
Adverse Reactions to Ibogaine Administration:
To start with we will look at existing data on reported fatalities (or near fatalities) related to consumption of Ibogaine.
Jamie Mac´s Study of 34 Adverse Reactions to Ibogaine
The ibogaine nurse Jamie Mac gave a presentation at the European Ibogaine Forum 2018 in which she presented 34 case studies of adverse reactions to ibogaine (many resulting in death) the following commonalities were observed
• 62% Sudden Cardiac Death / Acute Heart Failure Arrhythmias
• 35% Positive Toxicology (drugs in the system)
• 35% No cardiopulmonary disease history (although had other issues like electrolyte imbalance & toxicology etc)
• 29% Pre-existing cardiopulmonary disease
• 29% Self Administration
• 15% Liver disease
• 9% Psycho-Spiritual
• 3% Counterfeit Ibogaine
• 50% were Polysubstance Users
• 32% Cocaine / Crack / Speed users
• 29% Self-Administered
• 29% Alcohol users
• 23% Methadone
• 23% Benzodiazepines
Link to the article on Jamie Mac’s presentation: https://ibogainehotline.co/2018/12/15/ibogaine-safety-jamie-mac-ibogaine-cardiac-nurse/
Xaver Koenig and Karlheinz Hilber’s study of 19 Ibogaine Associated Deaths
In the scientific paper title “The Anti-Addiction Drug Ibogaine and the Heart: A Delicate Relation” published 2015, Koenig and Hilber of the Center for Physiology and Pharmacology at the Medical University of Vienna, studied the causes of 19 ibogaine related deaths and adverse reactions.
Between the years 1990 and 2008 a total of 19 fatalities associated with the ingestion of ibogaine were reported from which six subjects died of acute heart failure or cardiac arrest.
The found the following commonalities:
- 67% Long QT
- 50% Ventricular Tachycardia
- 33% Torsades de Pointes
- 33% Sudden Cardiac Death
- 17% Ventricular Fibrillation
Prolonged QTc intervals
- 75% QTc above 593
- 25% QTc between 480-498
Electrolyte imbalances:
- 100% Low Potassium
- 57% Low Magnesium
Other points of interest.
- In 14 of these cases adequate post-mortem data existed which demonstrated that almost all of the decedents suffered from pre-existing medical conditions or were compromised by the additional intake of other drugs such as opiates and cocaine
- Co-existing problems to do with the heart included: coronary artery sclerosis, hypertension, myocardial infarct, cardiac hypertrophy, and dilated cardiomyopathy
- Also some co-existing problems regarding the liver are mentioned such as hepatitis, liver cirrhosis and steatosis.
- No signs of neurotoxicity were found in these autopsies
Link to the article on this study:
Link to the original study:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4382526/pdf/molecules-20-02208.pdf
What do these Ibogaine Studies tell us?
They show us that there is a delicate relation between ibogaine and the heart. Almost all the deaths were related in someway to the heart.
Almost 30% of the subjects in Jamie Mac’s study had pre-existing cardiopulmonary disease and 35% had other drugs onboard which reacted badly with ibogaine causing the heart problems.
Koenig and Hibler’s study showed similar results with 74% of subjects showing that they either had pre-existing heart conditions or other drugs in their system which interacted with the ibogaine causing the deaths.
Possibly even more concerning is that 35% of the subjects in Jamie Mac’s study had no pre-existing cardiopulmonary disease history. Although in each of these cases there were electrolyte imbalances and other drugs in the system that caused the issues.
Most striking in Koenig and Hilber’s study is that 100% of the subjects had low potassium and 57% low magnesium. These electrolytes are vital for heart function. Hydration prior to ibogaine administration is considered vital and this study shows us why.
Stimulants drain electrolytes and also can cause a hyper excitable heart making stimulant users high risk. This is why most providers recommend that clients are off stimulants a week prior to arrival and it is extra important for stimulant users to hydrate well.
Ibogaine does not help with the physical withdrawal from alcohol or benzos. It can even make them worse and cause a Grand Mal Seizure. 29% of the people in Jamie’s study were alcohol users and 23% benzodiazpine users. It is important that alcoholics or the benzodiazipine dependent have been detoxed and are stable prior to ibogaine administration. The favoured method for benzodiazpine addiction is to stabilise on a set dose and continue that throughout the ibogaine treatment. That way they can detox from opiates (or other drugs) first and then, if they wish, do a long term slow benzo taper.
Ibogaine overdose or maladministration is potentially fatal. A high number of deaths were self administered ibogaine (29%). Proper guidance is needed to safety and successfully detox with ibogaine.
Methadone, subutex, suboxone and other long acting opiates are notoriously difficult to detox from with ibogaine and a topic of much discussion within the ibogaine community. Most providers recommend that users swap over to a short acting opiate like morphine or Oxycontin. This is because long acting opiates like Methadone stay in the system longer which makes overdose a higher risk (ibogaine makes opiates stronger), and also that the withdrawals tend to come back a few days later. There are providers who will detox people from these substances without swapping to a short acting opiate but they typically administer the ibogaine in a series of lower doses (to reduce risk of overdose) over a series of weeks or months to counter the reoccurring withdrawals. This is a controversial topic in the ibogaine community.
A case study of one person who detoxed straight from methadone with ibogaine was done by Clare Wilkins and ICEERS in Barcelona. It can be viewed here:
https://ibogainehotline.co/2017/12/09/detoxing-methadone-ibogaine-clare-wilkins-psychedelic-science/
It should be noted that this is just one test subject and more studies will need to be done to show whether this technique would work well on others.
What does Ibogaine do to the heart?
Ibogaine is a hERG channel blocker, and QT prolonging drug.
The hERG channel is best known for its contribution to the electrical activity of the heart: the hERG channel mediates the repolarizing IKr current in the cardiac action potential, which helps coordinate the heart’s beating.
When this channel’s ability to conduct electrical current across the cell membrane is inhibited or compromised, either by application of drugs or by rare mutations in some families, it can result in a potentially fatal disorder called long QT syndrome
The human body can handle a certain amount of hERG channel blockade and QTc prolongation, so for most peope this is not an issue. But for those with an already prolonged QT, electrolyte imbalances, QT prolonging drugs or other cardiac conditions it can cause fatal arrhythmia. Such as Ventricular Tachycardia, Ventricular Fibrillation, Torsades de Pointes and Cardiac Arrest / Death.
Because of this it is vital to monitor the QTc, blood pressure and pulse throughout an ibogaine treatment and to be able to administer the emergency care should it be needed.
Ibogaine can also cause bradycardia, tachycardia and raise and lower blood pressure.
On this page we will take a deeper look at each of these areas.
To see a full list of Medicines contraindicated by Ibogaine click here
Series of Events in Cardiac Events
The events regarding the cardiotoxicity associated with ibogaine appear to happen in the following order:
- Blockade of repolarizing hERG potassium channels;
- Retardation of the repolarization phase of the ventricular AP
- Prolongation of the QT interval in the ECG
- Paving the way for life-threatening Torsade de Pointes TdP arrhythmias.
Risks
Additional risk factors for drug induced TdP arrhythmias in a patient. These include:
- A prolonged QT
- Bradycardia / Tachycardia
- Abnormal electrolyte levels (in particular Low Potassium and Magnesium)
- Pre-existing heart disease
- Ion channel (e.g., hERG) mutations
- Drug-drug interactions
- Genetic variants influencing drug metabolism
- Female gender
For anti-addiction treatment with ibogaine these risk factors deserve special attention:
- Bradycardia (slow heart rate) Ibogaine itself induces bradycardia
- Hypokalaemia (Low Potassium).
- Hypokalaemia is frequent in drug users
- Drug-Drug Interactions
- History of poly substance use / stimulant use are at risk of “Hyper Excitable Heart Syndrome” which can cause Ventricular Arrhythmia
Due to the longevity of noribogaine—ibogaine’s active metabolite—in human plasma, cardiac adverse events may also occur several days, in some cases weeks after intake of a single dose of ibogaine. Noribogaine is believed to be important regarding the long-lasting anti-addictive effect of the treatment.
The use alongside ibogaine of a drug known to prolong the QT interval must be based on risk-benefit analysis.
The ibogaine-ascribed deaths occurred between 1.5–76 hours after drug intake. But ibogaine only has a half-life of only 4–7 hours so fatalities 24–76 hours after ingesting ibogaine cannot be attributed soley to the alkaloid. Also, QT interval prolongation after ibogaine administration typically lasts for more than 24 hours and has even been observed to occasionally last for longer than a week. Because of that it seems likely that noribogaine (which ibogaine converts to) constitutes the major cardiac risk rather than ibogaine itself.
Ibogaine should be administered under strict medical observation and continuous electrocardiographic monitoring for an extended time period, which carefully takes noribogaine’s longevity in human plasma into account.
Screening must include:
- A medical evaluation
- Physical examination
- ECG recording,
- Blood chemistry & electrolyte levels
- Haematological workup
- Psychiatric Report
- Chemical dependency evaluations.
In some cases, more extensive evaluations are required to rule out cardiac risk factors
Summary
In comparison to the many people who have received ibogaine treatments over many years worldwide, very few deaths have occurred or have been reported. In addition, drug safety studies on human addicts performed under well-controlled conditions revealed no significant adverse effects.
With the correct screening, preparation, intake, administration, observation by a trained team ibogaine can be deemed safe.
Cardiac monitoring demonstrated that no electrocardiographic abnormalities were produced or exaggerated following ibogaine administration in subjects that did not have any pre-existing cardiovascular risk factors.
Therefore it appears that ibogaine is well tolerated in drug-dependent subjects and implies that it is not ibogaine alone which causes these problems, but rather the drug in connection with one or more additional risk factors.
Xaver Koenig and Karlheinz Hilber
Further Information on Cardiac Conditions Related to Ibogaine
Sudden Cardiac Arrest / Sudden Cardiac Death
In Jamie Mac’s study 62% of ibogaine deaths were classified as either “Sudden Cardiac Death” or “Acute Heart Failure Arrhythmias”.
Sudden cardiac arrest (also known as cardiopulmonary arrest) occurs when the electrical system to the heart malfunctions and suddenly becomes very irregular. The heart beats dangerously fast. The ventricles may flutter or quiver (ventricular fibrillation), and blood is not delivered to the body sometimes so drastically that a person will lose consciousness. Death follows unless emergency treatment is begun immediately. Emergency treatment includes cardiopulmonary resuscitation (CPR) and defibrillation.
Sudden cardiac arrest is not a heart attack (myocardial infarction) but can occur during a heart attack. Sudden Cardiac Death is when the patient dies and Sudden Cardiac Arrest is when they survive.
Coronary artery disease is the most common cause of sudden cardiac death, accounting for up to 80% of all cases. Cardiomyopathies and genetic channelopathies account for the remaining causes (see list below). The most common causes of non-ischemic sudden cardiac death are cardiomyopathy related to obesity, alcoholism, and fibrosis.
Heart Attack or Sudden Cardiac Arrest: How Are They Different?
People often use these terms interchangeably, but they are not synonyms. A heart attack is when blood flow to the heart is blocked, and sudden cardiac arrest is when the heart malfunctions and suddenly stops beating unexpectedly. A heart attack is a “circulation” problem and sudden cardiac arrest is an “electrical” problem.
Common Causes of Sudden Cardiac Arrest
Ischemic Heart disease
- Myocardial infarction (Heart Attack)
- Anomalous coronary origin
- Coronary spasm (sudden tightening of the muscles within the arteries of the heart)
Inherited Channelopathies (Caused by disturbed function of ion channels or the proteins that regulate them)
- Long QT syndrome (LQTS)
- Short QT syndrome (SQTS)
- Brugada syndrome
- Early repolarization syndrome
- Catecholaminergic polymorphic ventricular tachycardia (CPVT)
- Electrolyte disorders
Cardiomyopathies (diseases that affect the heart muscle)
- Alcoholic
- Hypertrophic (a portion of the heart becomes thickened without an obvious cause)
- Idiopathic (Of unknown cause)
- Obesity-related
- Fibrotic (Pulmonary fibrosis is a lung disease that occurs when lung tissue becomes damaged and scarred)
- Arrhythmogenic right ventricular cardiomyopathy (ARVC)
- Myocarditis (inflammation of the heart muscle, can affect the heart’s electrical system)
- Drug toxicity (e.g., proarrhythmic effects of cardioactive drugs; epinephrine, cocaine, and related stimulants)
Heart Failure
- Nonpreserved ejection fraction (EF) systolic heart failure (EF less than 35%)
- Ejection fraction (EF) is a measurement, expressed as a percentage, of how much blood the left ventricle pumps out with each contraction. A normal heart’s ejection fraction may be between 50 and 70 percent.
Valve disease
- Aortic stenosis
Congenital diseases
- Tetraology of Fallot

Sudden Cardiac Arrest in relation to Ibogaine
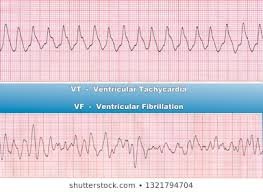
Ventricular Tachycardia (VT) and Ventricular Fibrillation(VF)
In Koenig and Hilber study of ibogaine deaths 50% had Ventricular Tachycardia and 17% had Ventricular Fibrillation
With ibogaine there is a risk of a lethal cardiac arrhythmia like “Ventricular-Tachycardia” or “Ventricular-Fibrillation”
These can lead onto a cardiac attack
They can be caused by many things (see below) but of particular interest in relation to ibogaine are; pre-existing heart disease, electrolyte abnormalities such as low potassium, certain medicines, and certain genetic diseases that affect the heart’s ion channels or electrical conduction.
This is because ibogaine causes (hERG) potassium channel inhibition and is known to prolong the QT interval.
Overdose of ibogaine, prolonged QT or electrolyte imbalances can put the patient at risk of VT and VF which can lead to cardiac arrest.
For this reason it is very important to monitor patients QT and QTc interval and get a full 12 Lead ECG EKG and blood panel showing electrolytes prior to admission.
ECG of Ventricular Tachycardia and Ventricular Fibrillation
Ventricular tachycardia (VT)
Ventricular tachycardia (VT) is a fast, abnormal heart rate. Starting in the heart’s lower chambers, called the ventricles. VT is defined as 3 or more ventricular contractions in a row at a rate of more than 100 beats a minute. If VT lasts for more than a few seconds at a time, it can become life-threatening. Sustained VT is when the arrhythmia lasts for more than 30 seconds, otherwise the VT is called non-sustained. The rapid heartbeat doesn’t give your heart enough time to fill with blood before it contracts again. This can affect blood flow to the rest of your body.
What causes VT?
VT is produced in two ways:
- An abnormal heart circuit within the ventricular muscle that is set in motion or triggered (called reentry)
- Abnormal ventricular muscle that becomes self activated (automatically)
VT can occur in an otherwise healthy, or structurally normal heart. It can also occur as a result of damage or scar in the heart from prior heart disease.
VT that occurs in the setting of structural heart disease is more concerning and often can be life threatening. VT that occurs in a structurally normal heart can be benign if it stops on its own.
Any heart condition that results in damage and scar to ventricular muscle can produce VT. It also be caused by an inherited arrhythmia such as long QT syndrome or Brugada syndrome.
VT is often linked to other heart problems that can damage or change normal heart muscle function. Damaged heart muscles can create abnormal electrical circuits that result in VT. You may be more at risk for VT if you have:
- Abnormal heart valves
- Cardiomyopathy
- Heart failure
- Coronary artery disease
- Heart attack
Some types of genetic diseases can also lead to VT. These include:
- Conditions that cause abnormal heart muscle, such as hypertrophic cardiomyopathy
- Diseases that can get inside the heart muscle, such as sarcoidosis
- Diseases that alter properties within the heart rhythm itself such as long QT syndrome or brugada syndrome
In some cases, VT occurs when there are no other heart problems.
Symptoms of VT
Fast beating heart that may only last for a few seconds. Longer episodes may be dangerous. The heart beats so fast that it struggles to get enough blood to the rest of your body.
Symptoms of VT include:
- Fast heartbeat or a fluttering feeling in the chest (palpitations)
- Dizziness
- Lightheadedness
- Chest pain
- Neck tightness
- Shortness of breath
- Fainting
- Cardiac arrest
In some cases, there are no symptoms at all
Treatment for sustained ventricular tachycardia
- Sustained ventricular tachycardia often requires urgent medical treatment, as may to lead to sudden cardiac death.
- Treatment involves restoring a normal heart using a defibrillator or with a treatment called cardioversion.
- Defibrillation can be done using an automated external defibrillator (AED).
- Cardioversion is done in a hospital setting using a machine that monitors your heart rhythm before and after shocks are delivered. In this procedure, medical professionals shock your heart using paddles, an automated external defibrillator (AED) or patches on your chest.
- There are also medications that can be used like Lidocaine (avoid amiodarone as it is QT prolonging). Be careful though as Lidocaine can kill someone in torsades.
Ventricular Fibrillation
Ventricular fibrillation (V-fib) is a dangerous type of arrhythmia, or irregular heartbeat. It affects the heart’s ventricles. In a healthy heart, your blood pumps evenly in and out of these chambers. This keeps blood flowing throughout your body.
Ventricular fibrillation is an arrhythmia that starts in your ventricle. This occurs when the electrical signals that tell your heart muscle to pump cause your ventricles to quiver (fibrillate) instead. The quivering means that your blood is not pumping blood out to the rest of your body. In some people, V-fib may happen several times a day. This is called an “electrical storm.”
Sustained V-fib can lead to sudden cardiac arrest (SCA) and/or sudden cardiac death (SCD). It needs immediate medical attention.
Causes of ventricular fibrillation
The cause of ventricular fibrillation is not always known but it can occur with certain medical conditions. V-fib most commonly occurs during an acute heart attack or just after. When heart muscle does not get enough blood flow, it can become electrically unstable and cause dangerous heart rhythms. A heart that has been damaged by a heart attack or other heart muscle damage is vulnerable to V-fib.
Other causes include heart failure, heart valve disease, electrolyte abnormalities such as low potassium, certain medicines, and certain genetic diseases that affect the heart’s ion channels or electrical conduction.
The most common risk factors include:
- A weakened heart muscle (cardiomyopathy)
- An acute or prior heart attack
- Genetic diseases such as long or short QT syndrome, Brugada disease, or cardiomyopathy
- Certain medicines that affect heart function
- Electrolyte abnormalities
Symptoms of ventricular fibrillation
Symptoms of V-fib include:
- Near fainting or transient dizziness
- Fainting
- Acute shortness of breath
- Cardiac arrest
How is ventricular fibrillation treated?
There are 2 stages of treatment for V-fib. The first tries to stops your V-fib immediately to restore a blood pressure and pulse. The second stage focuses on reducing your chances of developing V-fib in the future. Treatment includes:
- CPR. The first response to V-fib may be cardiopulmonary resuscitation (CPR). This will keep your blood moving to important organs.
- Defibrillation. This is an electrical shock that is delivered to the chest wall to restore normal rhythm. It is often critical to perform immediately once V-fib is diagnosed.
- Medicines Sometimes medicines are given immediately after V-fib to help control and prevent another episode.
- Implantable cardioverter defibrillator (ICD). This is a device that is implanted within the body to monitor for V-fib. If detected, it can automatically deliver an energy shock to restore normal heart rhythm.
“You need to know the difference between Ventricular Tachycardia and Torsades. The cure for V-TAC is lidocaine but will kill someone in Torsades”
― Dr Jeff Kamlet, Ibogaine Doctor
Torsades de Pointes – Most common rhythm
In the Koenig and Hilber study, out of 19 ibogaine deaths 33% had Torsades de Pointes
- Problems that occur with the heart’s rhythm are known as arrhythmias.
- When the heart beats faster than usual, as in a case of torsades de pointes, it is called tachycardia.
- Torsades de pointes is French for “twisting of points” and refers to when the heart’s two lower chambers (ventricles), beat faster than the upper chambers, which are known as the atria.
- Most cases of torsades de pointes resolve on their own without treatment. However, it can develop into ventricular fibrillation, which can lead to cardiac arrest and may even be fatal.
- Torsade de pointes is a distinctive form of polymorphic ventricular tachycardia (VT) characterized by a gradual change in the amplitude and twisting of the QRS complexes around the isoelectric line (see the image below).
- Torsade de pointes, is associated with a prolonged QT interval, which may be congenital or acquired.
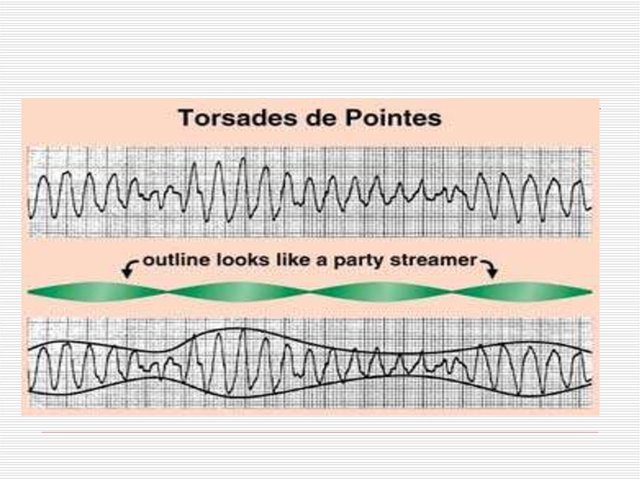
ECG of Torsades de Pointes
Common causes for torsades de pointes include drug-induced QT prolongation and less often diarrhea, low serum magnesium, and low serum potassium or congenital long QT syndrome. It can be seen in malnourished individuals and chronic alcoholics, due to a deficiency in potassium and/or magnesium.
-
Torsades de pointes — ‘twisting of the points.’ In this arrhythmia, your heart’s two lower chambers (ventricles) beat fast and chaotically, making the waves on an ECG monitor look twisted. Less blood is pumped out from your heart, so less blood reaches your brain, causing you to faint suddenly and, often, without any warning.
If a torsades de pointes episode is short — lasting less than one minute — your heart can correct itself and you regain consciousness on your own. However, if a torsades de pointes episode lasts longer, it can result in a sudden fainting spell followed by a full-body seizure. If the dangerous rhythm does not correct itself, then a life-threatening arrhythmia called ventricular fibrillation follows.
-
Ventricular fibrillation. This condition causes the ventricles to beat so fast that your heart quivers and ceases pumping blood. Unless your heart is shocked back into a normal rhythm by a defibrillator, ventricular fibrillation can lead to brain damage and sudden death.
It’s now known that long QT syndrome might explain some cases of sudden death
• TdP always requires ICU care.
• TdP is treated with IV Magnesium
Premature Ventricular Contractions (PVC) – a warning sign?
- PVCs may be a sign of a more dangerous heart rhythm to come.
- People with premature ventricular contractions get worse when they moved (to bathroom etc) or got agitated better to use a diaper or bowl
- Premature ventricular contractions (PVCs) are extra heartbeats that begin in one of your heart’s two lower pumping chambers (ventricles). These extra beats disrupt your regular heart rhythm, sometimes causing you to feel a fluttering or a skipped beat in your chest
- Purging often helps (vomit or defecate) with restoring electrical activity in the heart

Wide QRS
• Wide QRS complex tachycardia can be a sign of Ventricular tachycardia (VT) and Supraventricular tachycardia (SVT)
• A “wide QRS complex” refers to a QRS complex duration ≥120 ms. Widening of the QRS complex is related to slower spread of ventricular depolarization.
If you see a Wide QRS call emergency services (if recurrent)

Safety and Heart Resuscitation
• ACLS training is important! (Advanced Cardiac Lifesaver)
• Ibogaine can trigger an already unbalanced autonomic nervous system (speedballs do this as give both “rest” and “adrenaline” responses)
• The parasympathetic nervous system (PNS) controls homeostasis and the body at rest and is responsible for the body’s “rest and digest” function. The sympathetic nervous system (SNS) controls the body’s responses to a perceived threat and is responsible for the “fight or flight” response. Speedballs trigger both of these at the same time putting stress on the heart.
• Manual difibillator is best but you must know the correct joules for different cardiac conditions etc
• Difibillators with external pacing / use with benzo as painful contracts chest
• Pay attention to the patients Oxygen O2 as it should relate to the patients state (might drop during the deep trip for example)
• Learn all the heart algorithms check American heart association https://www.acls.net/aclsalg.htm
• Normally the person will feel bad
• Drug test everyone
• Get family medical history regarding the heart
• Ideal resus starts in first 3 mins with cardiac or respiratory arrest. To survive the goal is to have electricity in that heart in the first 3mins (defibrillator). Survival rates go down by 5% for every minute after
• Not good survival rates for out of hospital cardiac arrest 6-8% (because most aren’t noticed in time)
• Reoccurring episodes of torsades de pointes (TdP) require trans-venous pacing ICU (torsades is the most common rhythm)
• Trans-venous cardiac pacing, also called endocardial pacing, is used primarily to correct bradycardia. Transvenous pacing is achieved by threading a pacing electrode through a vein into the right atrium, right ventricle, or both.
• Torsades de Pointes (TdP) always requires ICU care.
• TdP is treated with IV Magnesium
• Ventricular Tachycardia is treated with Lidocaine (be careful though as Lidocaine can kill someone in Tdp)
• People have to sometimes get shocked above the QTc 600msc range (but usually only when other abnormalities are observed like a wide QRS)
• Ibogaine is never the reason for death alone, it’s always in combination with cardiac issues and toxicology (drugs in the system).
• Hidden Benzo dependence can cause seizures if benzos not stable throughout treatment
Blood Pressure
Ibogaine is known to both raise and lower blood pressure. So regular monitoring of the patients blood pressure is important.
Blood pressure chart for adults
top number (systolic) on the left side of the blood pressure chart. bottom number (diastolic) on the bottom of the blood pressure chart. Where the two meet is your blood pressure.

What blood pressure readings mean
As you can see from the blood pressure chart, only one of the numbers has to be higher or lower than it should be to count as either high blood pressure or low blood pressure:
- 90 over 60 (90/60) or less: You may have low blood pressure.
- More than 90 over 60 (90/60) and less than 120 over 80 (120/80): Your blood pressure reading is ideal and healthy. Follow a healthy lifestyle to keep it at this level.
- More than 120 over 80 and less than 140 over 90 (120/80-140/90): You have a normal blood pressure reading but it is a little higher than it should be, and you should try to lower it. Make healthy changes to your lifestyle.
- 140 over 90 (140/90) or higher (over a number of weeks): You may have high blood pressure (hypertension). Change your lifestyle – see your doctor or nurse and take any medicines they may give you. More on high blood pressure So:
- if top number is 140 or more – may have high blood pressure, regardless of bottom number.
- if bottom number is 90 or more – may have high blood pressure, regardless of top number.
- if top number is 90 or less – may have low blood pressure, regardless of bottom number.
- if bottom number is 60 or less – may have low blood pressure, regardless of top number.
QT Prolongation and Ibogaine
The QT interval is a measurement made on an electrocardiogram used to assess some of the electrical properties of the heart. It is calculated as the time from the start of the Q wave to the end of the T wave, and approximates to the time taken from when the cardiac ventricles start to contract to when they finish relaxing. In short its a way to monitor your hearts activity and health.
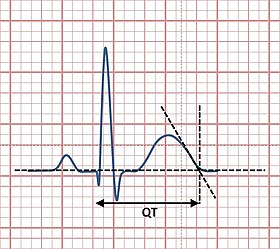
The picture above shows a normal QT, a prolonged QT would look as if it was “stretched out” when this happens there is a risk that the various parts of the heart may not fire in the right order, which can cause BIG PROBLEMS. See below:
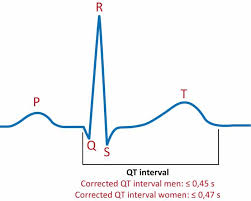
Need to correct the QT interval
The QT interval shortens at faster heart rates, and lengthens at slower heart rates. Since the QT interval is influenced by the heart rate, it needs to be corrected. A correction formula is required to come up with a corrected QT or QTc which estimates the QT interval at a heart rate of 60 beats per minute (bpm). This allows comparison of QT values over time at different heart rates.
What is the importance of the QTc?
The QTc, when prolonged means that the heart muscle takes longer than normal to recharge between beats. To have a prolonged QTc means one is at increased risk of arrhythmias, which when severe, can lead to syncope, cardiac arrest or sudden death. Prolonged QTc can be due to congenital defects, electrolyte imbalance, or medications
A QTc of >470 and >450 ms was associated with an increased risk of sudden death, for women and men, respectively, and a QT or QTc interval exceeding 500 ms can be regarded a significant risk for torsade de point. At least eight of such cases have been described in relation to ibogaine since 2008.
- QTc values ranged from minor prolongation of only 480 ms to a dramatic one with more than 700 ms in duration.
- Except for one case the prolongation of the QT interval subsequently evolved into ventricular tachycardia (VT) and/or ventricular fibrillation (VF). In many cases this developed into torsade de point (TdP) arrhythmias was observed.
- Only in one case the lack of arrhythmia occurrence was reported. However, in this case the QT interval was only minimally prolonged (480 ms).
In Koenig and Hilber study of ibogaine deaths 75% had a QTc above 593 and 25% QTc between 480-498
In all instances proper medical interventions could’ve saved the lives of these people.
Methods to correct the QT interval
There are four formulae to correct the QT interval, namely Bazett, Fredericia, Framingham and Hodges, of which Fredericia is the one we will use in the example below and is referred to as the QTcF or QTcFrid.
The QTcF may be arrived at manually or generated automatically by the ECG machine.
Below we will outline how you work out a QTcF manually.
Which ECG machine?
Some 12 lead ECG machines have an automatic QTc reporting feature and are preferred. But the QTc can still be worked out on a 3 lead ECG.33% Torsades de Pointes

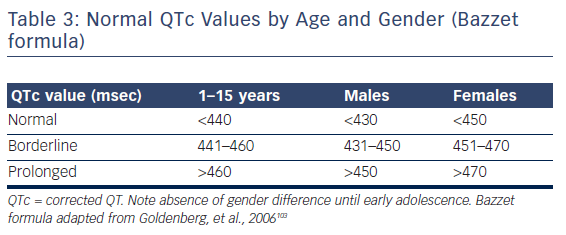
What values are considered abnormal QTc and what action is recommended?
The table below shows the normal and abnormal QTc (QTcF) values
- The WHO 2016 Guidelines consider a QTcF value of greater than 450 ms among males, or 470 ms among females, or an increase of 60 ms from baseline to be prolonged and requires that electrolyte testing and more frequent ECG monitoring be performed.
- A QTc interval of more than 500 ms is considered dangerous and is reason to stop the use of all QT prolonging drugs.
- If it goes above 600 get ready to use the AED Defibillator and get emergency services help.


The QT interval: the landmarks on Q and T are identified above.
- In practice, make an imaginary line on Q and on T on one heartbeat on the selected lead
- Count the number of small squares between Q and T: 8 small squares (in the example above)
- Multiply the number of squares by the unit time per square (0.04 sec): 8 small squares x 0.04
sec = 0.32 seconds
- Multiply the result by 1000: QT = 320 ms.
Note: In the example above, the ECG paper speed is 25 mm/sec. If the paper speed is 50 mm/sec the number of squares should be multiplied by 0.02.
There may be variations in the appearance of the QT interval.
Sometimes, a large U wave >1mm (supposed to follow the T wave) is fused to the T wave and should be included in the QT measurement.
Smaller u waves separate from the T wave should not be included. Sometimes, the T wave is notched. In this case, the maximum slope intercept method is used to define the end of the T wave, as shown below.
Strange T-Waves observed with Ibogaine
- T-Wave behaves very strangely on ibogaine, even going flat (inconsistent with being alive!)
- Cardiologists have seen nothing like it. Ibogaine is a very potent hERG blocker
- When flooded and ibogaine turns to noribogaine in the liver, the T wave changes appearance. Always disappear in less than 24 hours.



Multiply the number of small squares by the unit time per square (0.04):
20 small squares x 0.04 sec = 0.80 seconds.
The RR interval is 0.80 sec.
Note: In the example above, the ECG paper speed is 25 mm/sec. If the paper speed is 50 mm/sec, the number of squares should be multiplied by 0.02.
QTc (QTcF) Nomogram
Using the QTcF Nomogram below, locate the value of the QT interval obtained above (320 ms) on the first column of the Nomogram (indicated by the horizontal arrow) and the RR interval (0.80 s) or the heart rate (75 bpm) on the second row of the Nomogram (indicated by the vertical arrow).
Then find the value in the table that is common to both intervals (circled below). QTcF = 345 ms.

hERG channel
hERG (the human Ether-à-go-go-Related Gene) is a gene (KCNH2) that codes for a protein known as Kv11.1, the alpha subunit of a potassium ion channel. This ion channel (sometimes simply denoted as ‘hERG’) is best known for its contribution to the electrical activity of the heart: the hERG channel mediates the repolarizing IKr current in the cardiac action potential, which helps coordinate the heart’s beating.
- When this channel’s ability to conduct electrical current across the cell membrane is inhibited or compromised, either by application of drugs or by rare mutations in some families, it can result in a potentially fatal disorder called long QT syndrome.
- Also genetic mutations that increase the current through these channels can lead to the related inherited heart rhythm disorder Short QT syndrome.
- A number of drugs on the market inhibit hERG, lengthening the QT and potentially leading to a fatal irregularity of the heartbeat (a ventricular tachycardia arrhythmia called torsades de pointes).
- For this reason things that inhibit the hERG channel must be avoided.
- Patients must have sufficient Magnesium and Potassium levels to safely take ibogaine. A complete blood panel should show electrolyte levels. Too high potassium is also not good.
Altered Electrolyte Levels:
Hypokalemia (too little potassium) and often Hypomagnesemia (too little magnesium) are mentioned in case reports of ibogaine associated fatalities and cardiac arrhythmias (changes in heart rate).
In Koenig and Hilber’s study of ibogaine deaths 100% had Low Potassium and 57% had Low Magnesium
- Hypokalemia (low potassium) has a two-fold implication in generating long QT and an increased risk of TdP. Firstly it directly decreases hERG currents in the heart. Secondly it can also increase the blockade of hERG currents by drugs .
- Hypomagnesemia (low magnesium) was present in 57% of the case reports, and was always accompanied by hypokalemia. It is believed that also hypomagnesemia increases TdP risk
Drug-Drug Interactions
The addicted population is at high risk for adverse drug interactions.
- Several substances of abuse have been associated with hERG channel inhibition and/or QT interval prolongation. Especially alcohol, cocaine, and methadone. In combination with ibogaine there is a risk of a prolonged QT, and thus the risk of TdP arrhythmias will be raised.
- Methadone deserves special attention because it additionally has an exceptionally long plasma half- life (15–55 h)
- Ibogaine is metabolised to noribogaine mainly by the enzyme CYP2D6 (30% of most drugs are). Methadone inhibits CYP2D6 so it seems likely that this will impair the ibogaine.
- Since ibogaine’s active metabolite noribogaine has very similar cardiotoxic potential, drugs affecting noribogaine metabolism will be of relevance. Cardiotoxic effects may even persist for weeks after intake of a single dose of ibogaine.
Genetic Differences
Genetic variants with the CYP2D6 gene also need to be considered. People can be divided into different classes of metabolisers:
- Ultra-rapid
- Extensive
- Intermediate
- Poor
In poor noribogaine metabolizers, a single ibogaine dose may be enough to induce cardiotoxicity persisting for weeks.

Most of this website content was written by Rich Hughes, as well as the website creation itself.
In the photo to the left, he is the man on the right hand side.
He worked and volunteered for more than 5 years at various ibogaine detox clinics in México and Portugal before striking out on his own in Spain, his clinic is called Madera Sagrada which is Spanish for sacred wood, the indigenous Bwiti name for iboga.
During this time he has experienced the good, the bad and the ugly of ibogaine treatment; from the countless dozens who gained their freedom and even witnessing a death whilst working as a volunteer. This drove him to better understand the health and safety aspects, including how to read an ECG/EKG and an advanced first aid course.
It is with his hard won information, and a desire to see ibogaine knowledge distributed around the world, saving lives, as it has saved his life from Crack and heroin addiction.
"I´m just a common man who through his own experience and desire has studied ibogaine and iboga and their correct administration. I stand on the shoulders of giants and through my web and graphic design skills I´ve decided to disseminate this info to a wider audience, with the hope of spreading liberty to those that desire it
www.maderasagrada.org
maderasagrada@protonmail.com
+34 643280060 (Whatsapp & Telegram available)
Learn about the jaw-dropping benefits of Ibogaine and Iboga. They do so much more than just addiction treatment
Ibogaine can be dangerous for some people. Educate yourself to see if you are a good candidate for this work
Preparing for your iboga ceremony or ibogaine treatment. Mentally, emotionally, physically and spiritually.
Learn what medication and medical health conditions are a bad mix with ibogaine and iboga.
Make sure you go to a good place! There are some shady operations going on out there…
Ibogaine and the heart have a delicate relationship. Indepth article about the action on the heart.

Talk to us!
Our knowledgeable volunteers will share their personal experience of ibogaine with you and advise you on how to find a good clinic.
+34 643280060
For a free call back:
Text, Whatsapp, Telegram app or email us!
brain@ibogainehotline.co
Or by clicking the blue speech bubble to the right of the screen to chat to us right now!
Join our facebook group and get first hand advice from people who have already made their journies with ibogaine www.facebook.com/groups/1521724148001426/
Like our Facebook page www.facebook.com/ibogainehotline

We wish you luck on your journey. This incredible medicine has changed so many lives, but to do safe and effective work it must be treated with respect.
It’s important that you find a good provider or clinic to do your ibogaine treatment with. Don’t end up with the cowboys!
We do our best to keep this website updated as our collective knowledge and experience of the use of ibogaine grows, and we would love you contributions and suggestions. Email us

The Anti-Addiction Drug Ibogaine and the Heart: A Delicate Relation
Read More

Entheo-Science – Jeff Kamlet: Ibogaine Safety
Read More

Detoxing from Methadone with Ibogaine – Clare Wilkins Psychedelic Science Conference 2017
Read More

Dr Fred’s Ibogaine Safety Presentation at the European Ibogaine Forum
Read More

Ibogaine Adverse Reactions & Safety – Jamie Mac – Ibogaine / Cardiac Nurse – Notes from the European Ibogaine Forum
Read More

Welcome to Ibogaine Hotline
Read More

Dutch study on the longterm benefits of ibogaine treatment for drug addiction
Read More